OUR SERVICES
OUR SERVICES
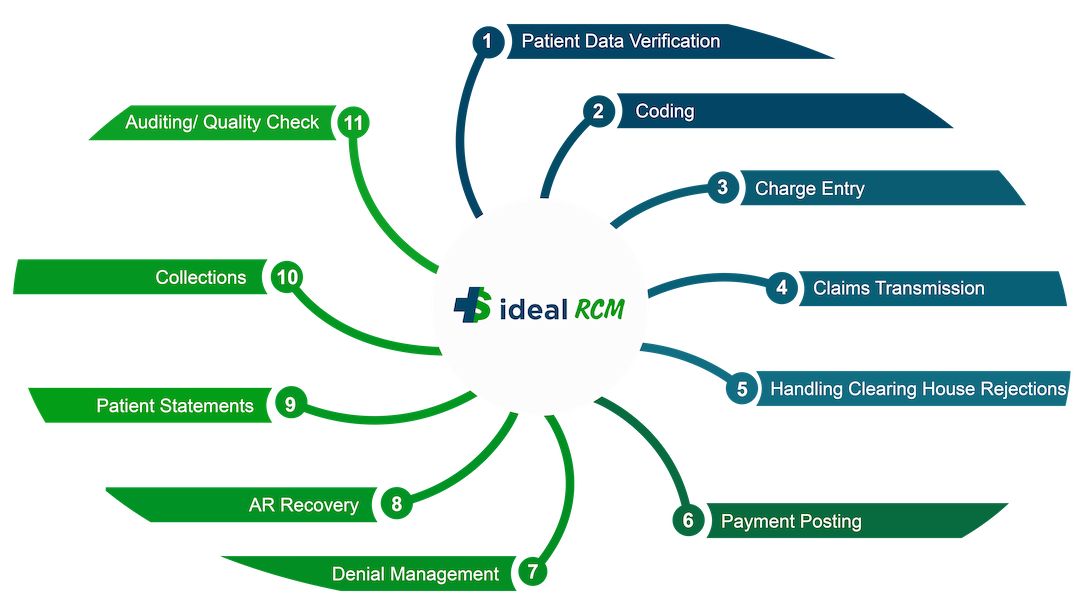
Patient Data Verification
Coding
Charge Entry
Claims Transmission
Handling Clearing House Rejections
Payment Posting
Denial Management
AR Recovery
Patient Statements
Collections
Auditing/ Quality Check
Patient data verification
Patient registration is one of the most important aspects of your revenue cycle. Your patients’ data isn’t only important for medical records, but it also has a significant impact on the payment of insurance claims. And thus, it is crucial to have an error-free patient registration process. Our team of highly skilled personnel verifies required patient data for processing Claims including demographics and insurance information, entered during the registration. This facilitates quick claims processing, reduces claim denials, and helps you get paid on time.
Coding
We offer the best medical coding service in the industry to all our clients. We help you comply with government regulations and industry standards. Our team of experienced coders are up to date with the current standards. They accurately code all the medical services made available to your patients and ensure that your claims are reimbursed timely.
Charge Entry
Charge entry is the process of ensuring the accuracy of medical coding, patient demographics, insurance information, physician information, date of service, place of service, type of service, etc. before submitting the claim. A meticulous charge entry process helps you improve your revenue cycle and reduce late payments and claim rejections. Any mistake or discrepancies in your medical coding can result in claim rejection and payment delays.
We have a dedicated team of charge entry experts who process a large volume of charge entries with high precision. With their expertise and our cutting-edge technology, you’d be able to witness a phenomenal growth of your revenues.
Claims Transmission
Claims transmission is another extremely important step in the medical billing process.
At Ideal RCM Medical Billing, we offer you a full-fledged claims transmission service. Our team of auditors thoroughly reviews the forms and makes corrections wherever before this step. We help transmitting the claims to the clearing house or directly to the payer of your choice.
Handling Clearing House Rejections
Sometimes even when you think you did everything correctly, your claims can still get rejected by the clearinghouse. Claim rejections usually happen due to errors in insurance information or specific insurance requirements. Once rejected, you have the chance to deal with the issues, make corrections and re-submit your claim to the insurance company.
At Ideal RCM Medical Billing, we help you handle clearinghouse rejections effectively. Our team pays a great deal of attention to your rejected claims. We analyze every detail and provide you with an accurate and error-free rejection resolution.
Further, we deliver our rejection handling service at a super-quick turnaround time so that there is no further delay, and you can get your reimbursements as soon as possible.
Payment Posting
We provide our clients with a cost-effective and quick payment posting service. We make sure to handle all your payment posting requirements in the best possible manner. We help you accurately post the insurance payments to your patient’s account.
Our team can go through and analyze the EOBs (explanation of benefits) and ERAs (electronic remittance advice) at an exceptionally rapid pace. This helps us deal with cases of co-insurance, uncovered insurance, etc., and provide you with quick and accurate logging of payments in your billing software.
Denial Management
At Ideal RCM Medical Billing, we understand the importance of timely denial resolution. And thus, we are completely dedicated to ensuring that you can reap all the benefits of our extensive denial management solution.
We have a team of denial analysts who have extensive experience in the industry. They assist you in identifying the root cause of claim denial and take every possible step to resolve the issues. Our key denial management services include:
- Accurately identifying the reason and source of claim denials
- Detecting patterns and trends of denials
- Resolving the issues and improving your revenue cycle
- Resubmission of denied claims
Providing detailed reports and feedback to our client
AR Recovery
With our effective AR recovery process, you’d be able to realize your net collections to their full capacity. We have a team of professionals who specialize in the AR recovery and follow-up domain. They provide you and your organization with systemized and streamlined AR recovery solutions.
Our team helps you in effectively collecting your outstanding amount in three steps:
- We perform an initial evaluation of the claims listed in your AR aging documents
- We then identify the “uncollectible” claims
- After a thorough analysis, our team identifies the claims that are within the re-filing range. We then precisely verify all the information and re-file the collection claims
Patient Statements
We generate detailed patient statements every week on a 30-day cycle to ensure that everything is up and running. We send the statements to each of your patients on time as specified by your practice and mention our contact number on it.
This way, if your patients have any questions regarding their bills or the amount they must pay, they can directly contact us. This frees up a lot of your valuable hours and you won’t have to deal with a single phone call. From answering your patients’ questions to interpreting their EOBs, we take care of everything for you.
Collections
Ensuring that you receive every single penny you rightfully deserve is our top priority. We make every possible effort to collect your money and help you get paid on time.
We send multiple patient statements and contact your patients via phone to help them settle their bills on time. Our persistent follow-up techniques ensure that you don’t have any unpaid or outstanding amounts. Our team regularly monitors your payments, and if a patient still has an outstanding amount, we take your approval and turn it over to a collection agency you get reimbursed on time.
At Ideal RCM Medical Billing, your success is our responsibility.
Auditing/ Quality Check
With our auditing and quality check services, you can improve the accuracy of your insurance claims, identify, and solve compliance issues. Moreover, we work with your team to help you recover your lost charges and avoid all kinds of costly mistakes while submitting your claims.
We have a well-established analytical approach that helps us in verifying and validating all the written documents in our client’s system. Our team of skilled auditors runs a thorough check on all your claims-related paperwork to identify coding mistakes, occurrences of undercharges, duplicate postings, etc.
